All published articles of this journal are available on ScienceDirect.
Effect of the Fraction of Inspired Oxygen on Intermittent Central Venous Oxygen Saturation Measurements
Abstract
Background:
Central venous oxygen saturation (ScvO2) is an essential test readily performed both by medical and nursing personnel in a critical care setting. It gives information on the patient‘s oxygen supply, oxygen consumption, and cardiac output. It plays an important role in early goal-directed treatment.
Objectives:
This study was planned to assess the effect of different fractions of inspired oxygen (FiO2) levels on central venous oxygen saturation for consideration during the evaluation of central venous oxygen saturation.
Methods:
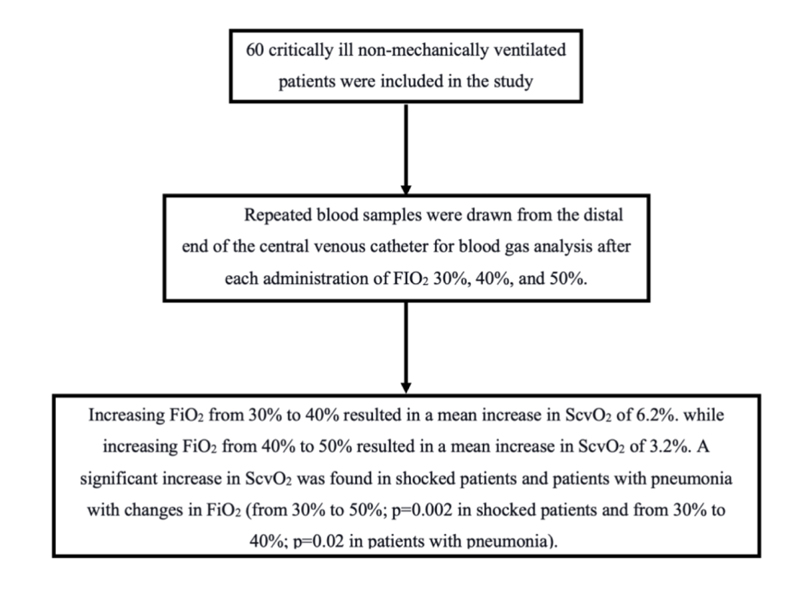
This interventional cross-over study enrolled 60 critically ill, nonmechanically ventilated patients. Blood samples were repeatedly drawn from the distal end of the central venous catheter for blood gas analysis after administration of 30%, 40%, and 50% FIO2 respectively.
Results:
The results showed that increasing FiO2 from 30% to 40% resulted in a mean increase in ScvO2 of 6.2%. While increasing FiO2 from 40% to 50% resulted in a mean increase in ScvO2 of 3.2%. A significant increase in ScvO2 with changes in FiO2 levelwas recorded among patients in shock or patients with pneumonia (from 30% to 50%, p=0.002 in shock patients and from 30% to 40%, p=0.02 in patients with pneumonia).
Conclusion:
Increasing FiO2 resulted in a substantial rise in ScvO2. ScvO2 changes in response to a therapeutic challenge should be interpreted at constant FiO2 level, especially in patients with pneumonia.
1. INTRODUCTION
The oxygen content of blood returning to the right side of the heart after perfusing the entire body is measured by venous oxygen saturation (SvO2) [1]. The hemoglobin saturation of blood in the superior vena cava and proximal pulmonary artery is referred to as central (Scvo2) and mixed venous oxygen saturation (SvO2), respectively [2]. ScvO2 is a vital measurement that can be performed by medical and nursing personnel in a critical care setting. It provides an understanding of the patient‘s oxygen delivery, oxygen consumption, and cardiac output [2]. When taken and evaluated properly, it plays an important role in the early goal-directed treatment and has been associated with reduced mortality [3]. A ScvO2 > 70% or mixed venous oxygen saturation (SvO2) >65% is indicated for septic and non-septic patients. [4]
Shock is defined as global cellular and tissue hypoxia secondary to either decreased systemic oxygen delivery (DO2), systemic oxygen consumption (VO2), inadequate oxygen utilization, or combined. A decrease in DO2 is compensated for by an increase in VO2, thereby preventing tissue hypoxia. Tissue hypoxia and lactic acidosis begin when a ‘critical’ DO2 level is reached, and no more oxygen can be taken [1]. Untreated tissue hypoxia is associated with an increase in morbidity and mortality [5]. Therefore, an accurate diagnosis of global tissue hypoxia is critical. Physical examination, vital signs, measurement of central venous pressure, and urine output are all relevant but are still insufficient for detecting global tissue hypoxia [5].
The measurement of mixed venous oxygen saturation in the pulmonary artery (SvO2) has been recommended as an indirect indicator of tissue oxygenation. However, the use of the pulmonary artery catheter has become somewhat unpopular. By contrast, insertion of a central venous catheter into the superior vena cava is considered standard care in critically ill patients. The assessment of central venous oxygen saturation (ScvO2), similar to SvO2, has been recommended for detecting global tissue hypoxia [5, 6].
ScvO2 levels can be monitored on an as-needed basis (intermittently) by taking blood from the central line for blood gas analysis. It may also be monitored in real-time (continuously) using a fiberoptic catheter equipped with reflection spectrophotometry. The saturation level is shown on an oximetry meter and is updated every 2 seconds [1].
Cardiac output, plasma hemoglobin concentration, blood transfusions, and blood volume are the most important factors influencing ScvO2 and may lead to misinterpretation of SCvO2. [7]. Therefore, this study was planned to assess the effect of different fractions of inspired oxygen (FiO2) levels on central venous oxygen saturation for consideration during the evaluation of central venous oxygen saturation.
2. MATERIALS AND METHODS
This interventional cross-over study included 60 critically ill, nonmechanically ventilated patients admitted to the respiratory critical care unit of the Chest Medicine Department at Mansoura University. All included patients already had a central line. This study was conducted within the required ethics guidelines of the Mansoura Institutional Research Board ethics committee (code number: R.21.10.1485). Informed written consent was obtained from the included patients.
Blood samples were repeatedly drawn from the distal end of the central venous catheter for blood gas analysis. The samples were aspirated into a heparinized blood gas syringe 30 min after administration of 30%, 40%, and 50% FiO2 respectively. The samples were then analyzed in a blood gas analyzer, which was regularly calibrated.
Statistical analysis of the data was performed using SPSS V.16. A repeated-measure ANOVA with a Greenhouse-Geisser correction and post hoc tests using the Bonferroni correction were conducted.
3. RESULTS
A total of 60 patients (mean age 61±11 years) were included in the study. Males represented 58.6% (35) of the patients. In total, 37.9% of the patients had pneumonia, and 19% were hemodynamically unstable (Table 1). A subclavian catheter was inserted in 27 patients, and 33 patients had jugular catheters. All patients were spontaneously breathing, and oxygen was delivered via a simple facemask. We recorded ScvO2 after 30 min of each increase in the FiO2.
| - | No | Percent (%) |
|---|---|---|
| Gender: Male Female |
35 | 58.6 |
| 25 | 41.4 | |
| Shock | 11 | 19.0 |
| Anemia | 21 | 36.2 |
| Pneumonia | 22 | 37.9 |
| age | mean± SD | 61.6± 11 |
The results of this study showed that increasing FiO2 from 30% to 40% resulted in a mean increase in ScvO2 of 6.2%, whereas increasing FiO2 from 40% to 50% resulted in a mean increase in ScvO2 of 3.2%. A repeated-measures ANOVA with a Greenhouse-Geisser correction determined that the mean ScvO2 differed significantly between different levels of FiO2 (F (1.710, 83.8) = 9.23, p < 0.001). Post hoc tests using the Bonferroni correction revealed a statistically significant increase in ScvO2 when FiO2increased from 30% to 40% (64.7 ± 15.85 vs. 70.998 ± 13.8, p=0.011) and from 30% to 50% (64.7 ± 15.85 vs. 74.098 ± 10.19, p = 0.003). However, the increase in ScvO2 when FiO2was changed from 40% to 50% (70.998 ± 13.8 vs. 74.098 ± 10.19, p = 0.33) was insignificant (Table 2).
| - | Mean | Std. Deviation | F | Significance | Partial Eta Squared |
|---|---|---|---|---|---|
| ScvO2 30b,d | 64.7500 | 15.85000 | F (1.766, 83.8) = 9.230 | <0.000 | 0.159 |
| ScvO2 40b,c | 70.9980 | 13.84906 | |||
| ScvO2 50c,d | 74.0980 | 10.19781 |
A significant increase in ScvO2with changes in FiO2was found among patients in shock and those with pneumonia (from 30% to 50%; p = 0.002 in shock patients and from 30% to 40%; p = 0.02 in patients with pneumonia). However, a nonsignificant increase in ScvO2 was found when FiO2 was changed in hemodynamically stable and anemic patients and in those without pneumonia (Table 3).
Table 3.
| Factor | scvo30 mean (SD) |
scvo40 mean (SD) |
scvo50 mean (SD) |
F | Overall Significance | Pairwise Significance | Partial Eta Squared |
|---|---|---|---|---|---|---|---|
| Shock | 51(14.4) a | 59.8 (11.1) | 72.8(8.5) a | F (2,16) =14.2 | <0.001 | a= 0.002 | 0.639 |
| No shock* | 67.3 (15.9) | 73 (14.1) | 72.6 (11.2) | F (1.6,48.4) =2.02 | 0.152 | 0.06 | |
| Anemia | 63.4 (19.7) | 69.5 (17.4) | 74.2 (12.4) | F (2,34) =2.7 | 0.08 | 0.138 | |
| No anemia* | 64.2 (14.6) | 70.5 (11.9) | 71.3 (8.9) | F (1.6,33.5) =3.27 | 0.061 | 0.135 | |
| Pneumonia | 60.1 (14.5) a | 65.9 (9.2) a | 70.5 (10) | F (2,34) = | 0.005 | a=0.029 | 0.269 |
| No Pneumonia | 66.9 (17.5) | 74.1 (16.4) | 74.4 (10.5) | F (2,46) =2.2 | 0.12 | 0.088 |
4. DISCUSSION
Proper hemodynamic monitoring of critically ill patients is still in some way challenging.
ScvO2 represents a surrogate parameter for the evaluation of the O2 demand/supply adequacy. Therefore, there is extensive interest in the utilization of ScvO2 to guide fluid and inotrope administration [8]. A previous study by Rivers et al. [9] on septic patients revealed a decline in morbidity and mortality in the early goal-directed therapy in which ScvO2 was adjusted to more than 70%. In addition to cardiac output, ScvO2 is also affected by a range of factors that affect blood oxygen content and tissue oxygen consumption. The effects of changing FiO2 levelson ScvO2, i.e. the highlight of the present study, were not considered by Rivers et al. [9].
The results of this study showed that increasing FiO2 from 30% to 40% resulted in a mean increase in ScvO2 of 6.2%, while increasing FiO2 from 40% to 50% resulted in a mean increase in ScvO2 of 3.2%. Jee and White [10] also investigated the effect of increasing FiO2 to 100% on ScvO2 in critically ill patients and found that the mean increase in ScvO2 was 6.7%.
Nam et al. [ 11 ] reported that SvO 2 increased by ≥5% in more than three-quarters of FiO 2 increases from 30% to 80% or 50% to 100% during cardiac surgery and by ≥10% in the remaining one-quarter of FiO 2 changes. Whereas HB remained almost fully saturated, PaO2 changed remarkably as FiO2 was changed. Legrand et al. [7] concluded that PaO2 should not be overlooked while considering the ScvO2 value as a therapeutic goal, as the author’s observed that ScvO2 rose from 71% to 83% after increasing FiO2 [7].
In patients with or without anemia, a nonsignificant increase in ScvO2 was found with changing FiO2 in this study. This result is compatible with that of Nam et al. [11], who found a nonsignificant association between Hb concentration and ΔSvO2.
A significant increase in ScvO2 with changes in FiO2 was found among patients in shock and those with pneumonia in this study. This observation may have significant implications for the interpretation of ScvO2 data in clinical practice. However, the cause of the shock was not identified in this study.
CONCLUSION
Increasing FiO2 was linked to a substantial rise in ScvO2, which would consequently affect the interpretation of ScvO2 data. Interpretation of variations in ScvO2 in response to a therapeutic challenge should be performed at constant FiO2, especially in patients with pneumonia.
LIST OF ABBREVIATIONS
| ScvO2 | = Central Venous Oxygen Saturation |
| FiO2 | = Fractions of Inspired Oxygen |
| DO2 | = Decreased Systemic Oxygen Delivery |
| VO2 | = Systemic Oxygen Consumption |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
This study was conducted within the required ethics guidelines of the Mansoura Institutional Research Board Ethics Committee, Egypt (code number: R.21.10.1485).
HUMAN AND ANIMAL RIGHTS
No animals were used for the studies that are the basis of this research. This research was conducted on humans in accordance with the Helsinki Declaration of 1975, as revised in 2013 (http://ethics.iit.edu/ecodes/node/3931).
CONSENT FOR PUBLICATION
Informed written consent was obtained from included patients.
STANDARDS FOR REPORTING
STROBE guidelines and methodology were followed.
AVAILABILITY OF DATA AND MATERIALS
The data supporting the findings of the article are available within the article.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


